People
Topics
Share
For employers with robust benefits programs in place, an integrated approach is continuing to become an increasingly popular way to take things to the next level, and for good reason. Although the concept is not new, and our team of experts has been developing solutions for years, certain aspects are getting employers’ attention.
Spring’s 2016 and 2018 employer surveys, led by Spring’s Senior Vice President Karen English, show that the core drivers to developing an integrated program are:
- Costs savings
- Simpler administration
- Upgraded employee experience
- Enhanced tracking capabilities
- Improved compliance
There’s a lot more impacting these areas than you might think, so let’s take a deeper dive.
Cost Savings:
Having an efficient benefits program with systems that speak to and work with each other can go a long way for your bottom line. Integration provides greater transparency into your workforce – absence management challenges, productivity, employee health – among other things. This knowledge is an opportunity to create a healthier, more present workforce.
If this sounds like qualitative “fluff”, it’s not. One healthcare client was able to save over $10M in direct and indirect costs through integration. These savings resulted from savings in the following areas:
- Workers’ compensation
- Disability
- Unplanned absence
- Vacation
- Other Leaves of Absence
Their program, done in tandem with captive insurance company funding, also yielded risk diversification and stability, as well as further savings of 10% of premiums.
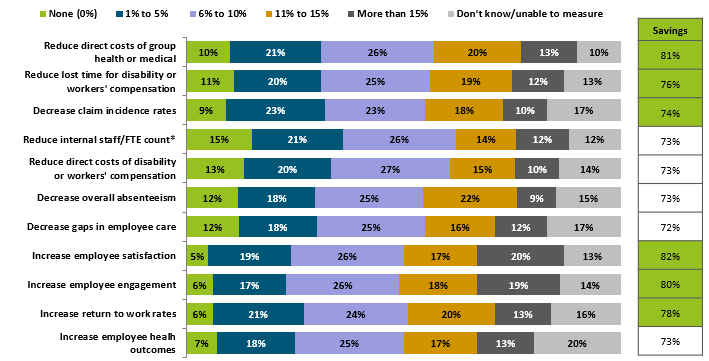
The graph below shows the average levels of employer savings achieved by implementing an integrated program, spanning a range of direct and indirect cost categories.
Simpler Administration:
All parties benefit from an integrated benefits system. An immeasurable amount of time and effort is saved from not having to go to different platforms for critical information. This will speed up the claims process.
The best integrated programs send notifications and communications, and offer automated triggers, case management and documentation. For managers, results are easier to explain. For employees, access is simpler and more approachable. At the corporate level, you can expect faster turnaround time and greater visibility.
Upgraded Employee Experience:
Employees do not typically understand the nuances surrounding absences, nor the various policies, plans, and processes involved. They simply need time away. By integrating absence to include occupational and non-occupational events, your employees will experience:
- Fewer points of contact
- Clearer processes to follow
- Faster turnaround times
- Improved information access
- Increase self-service options
- Decreased confusion
These benefits lead to an enhanced employee experience including higher engagement, both at the organization and with their health. As all HR professionals know, engagement is critical for recruiting, retention and overall performance. Whether at risk or not, all employees will appreciate a smarter, more robust benefits program and an employer that is looking out for their wellbeing.
Enhanced Tracking Capabilities:
To make sustainable improvements, it is imperative to track your integrated program and mine the data across all absences to investigate patterns and draw predictions. An integrated program allows for metrics across plans and policies with drill-down features such as:
- Occupational vs. non-occupational
- Paid vs. unpaid
- Job protected vs. non job protected
- Return-to-work vs. stay-at-work
- Sick, vacation, etc.
- Self vs. family
- Continuous vs. intermittent
- Diagnosis specific
With all these different facets captured uniformly, you have reporting that is comprehensive; supports workforce planning and budget; allows for strategic planning with HR as a business partner; and offers opportunities for prevention; so that your organization can be proactive instead of reactive. These kinds of insights allow employers to move into population health management.
Improved Compliance:
With the hub of intelligence that an integrated program offers, employers have a more reliable way of remaining compliant when it comes to things like the ADA, FMLA and ERISA, as well as any state-specific regulations and policies unique to the company. Automation will make leave requests and absence tracking much easier to manage, and accurate documentation will aid accountability for employers and employees alike.
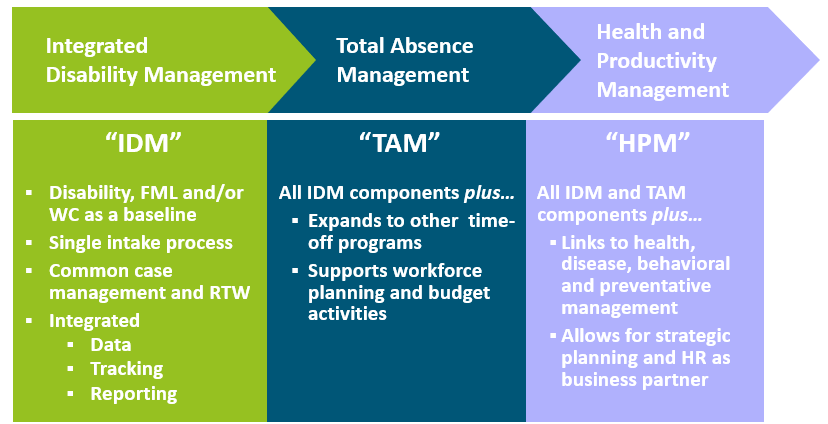
Ultimately, an integrated workers’ compensation and disability program can have significant positive impact on a company and its employees, especially for larger employers. We have seen great, quantifiable success with integrated programs from our clients. If you are thinking that this process seems too big a task to take on, don’t worry. Any company can start at any point along the continuum shown below, and gradually work their way to a model that facilitates population health management in the workforce.
Most Common Approach is Phased